A cancer diagnosis is a life-changing event that sends ripples through the lives of patients and their loved ones. Radiation oncologist Dr. Brian Baumann says Washington University researchers are working to lessen the burden by making cancer treatment easier on the patient. One of the university’s most promising fields of study is proton therapy, which can offer reduced side effects and a better quality of life.
Baumann, who is based at Siteman Cancer Center at Barnes-Jewish Hospital, was the lead author on a recent study suggesting that proton therapy is less likely to cause nausea, vomiting, diarrhea and dehydration than traditional X-ray radiation. This means that fewer patients become ill and end up back in the hospital after treatment. The study, a partnership between Washington University School of Medicine and the University of Pennsylvania, included 1,500 patients with cancers of the brain, head, neck, lung, digestive tract and female reproductive system. They were treated with combinations of chemotherapy and either X-ray radiation or proton therapy.
“In the X-ray radiation group, 27.6% of patients experienced a severe side effect in the 90 days following treatment, but in the proton therapy group, that figure was 11.5%,” Baumann says. “Patients in the proton therapy group had a two-thirds reduction in their relative risk of severe side effects in that time period.”
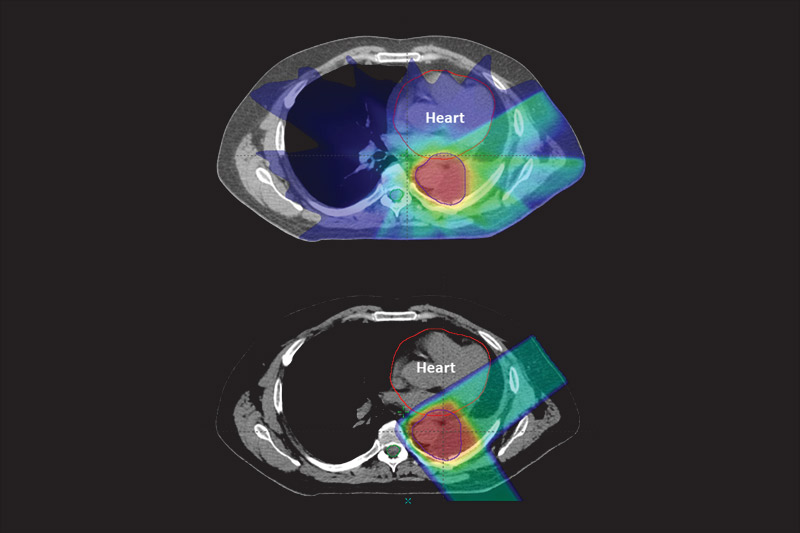
Proton therapy isn’t new, but it’s now being recognized as a promising alternative to deliver radiation treatment to a cancerous growth, Baumann explains. It uses a beam of protons to target diseased tissue and differs from traditional radiation because it doesn’t go beyond the tumor and into the surrounding tissue. “Because of proton therapy’s reduced toxicity, we likely will be able to increase doses beyond what we can give with traditional radiation, which should improve cure rates,” he says.
Another plus, Baumann says, is that people receiving proton therapy are able to do more of their normal daily activities because they don’t feel as ill during treatment. “We look at patients’ ‘performance status,’ a measure of their functional capabilities, and that seems to be affected less by proton therapy,” he says. “Many people can continue working while they’re in treatment, and that’s a big advantage.”
Baumann says proton therapy usually is delivered in a hospital setting. Siteman currently has one proton therapy system and plans to add another this summer. “At Washington University, we have been treating cancer with the current technology since 2013, so we have a lot of experience with it,” he says.
According to Baumann, more research on this topic is in the works. “Additional studies are looking at results, other possible applications, other disease sites and questions about cost-effectiveness,” he says. “It’s not clear yet if proton therapy could replace traditional radiation, but it’s very promising. It’s likely that the cost of the therapy will come down eventually, and if it continues to be supported by evidence, we should be able to treat more patients and gain a bigger data set to help us evaluate effectiveness. Proton therapy isn’t appropriate for everyone, but its potential for fewer side effects and better quality of life is something patients should consider.”
Image: Dr. Brian Baumann, Mike Worful